 Let’s not forget all the men with hypothyroidism.
Let’s not forget all the men with hypothyroidism.
Written by David Borenstein, MD
When it comes to hypothyroidism – an underactive thyroid – we usually think of women. Women, after all, are at least eight times more likely than men to develop thyroid problems. This explains why so much of the information, advocacy, websites, and research are focused on thyroid problems in women, versus men.
But that doesn’t mean that men can’t develop an underactive thyroid. As an integrative physician, I treat men all the time who have been struggling with a host of symptoms that end up being diagnosed as hypothyroidism.
So I’d like to start by thanking incredible patient advocate, Dana Trentini, for this opportunity to reach out on her Hypothyroid Mom blog to share information not only with all you Hypothyroid Dads out there, but any men with an underactive thyroid who may be struggling to get diagnosed or properly treated.
Getting Diagnosed
The symptoms of hypothyroidism in men are similar to those in women. Some of the most common include exhaustion, weight gain, and depression. Other common symptoms include feeling cold, constipation, muscle aches and pains, and low resistance to infection. These are not all the symptoms, by any means. They’re just the tip of the iceberg. For a comprehensive list, check out Dana’s 300+ Hypothyroidism Symptoms…Yes REALLY.
There are symptoms, however, that seem to be more common in men. Some of you may find you aren’t gaining weight, but are losing muscle, as well as muscle strength. You may also notice a concerning drop in your sex drive. Or the first sign of a thyroid issue may be premature balding or rapid shedding of your hair (including eyebrows and body hair.)
If any of these symptoms sound familiar, the first stop is your doctor.
One up-front warning: Do not let your doctor tell you that these are common symptoms for “men your age”, that you just need more sleep or exercise, that only women get thyroid problems, and don’t just accept a prescription for an antidepressant. Insist on having thyroid testing.
Many conventional physicians will only want to run one test, called the Thyroid Stimulating Hormone – or TSH – test. Time to push back, and insist on a more comprehensive thyroid panel, including Free T4, Free T3, Reverse T3, and Thyroid Peroxidase Antibodies (TPO), at minimum. This panel will tell you the pituitary’s response to your thyroid (the TSH test), the circulating levels of actual thyroid hormone (Free T4 and Free T3), whether you are producing an ineffective form of thyroid hormone (Reverse T3), and whether you have antibodies that suggest you have Hashimoto’s disease. Hashimoto’s is an autoimmune disease — think of it as the immune system shooting friendly fire against your own thyroid gland — that is the most common cause of hypothyroidism in the U.S.
Your first challenge: Don’t accept “normal” as a result for your thyroid test. At most labs, the reference range for the TSH test is from around .5 to 5.0. The problem is, many doctors deem any test result within that range as “normal.” But in my practice, I’ve found TSH levels less than 2.0 to reflect adequate thyroid function. But if all you hear is “your thyroid tests were normal” – without knowing the actual number – you won’t know that your TSH above 2.0 may be indicative of low-level hypothyroidism.
Your second challenge: The TSH test is not infallible, and it can miss situations where the actual levels of thyroid hormone are not sufficient. So make sure your doctor runs the Free T4 and Free T3 levels, and gives you not only the results, but the reference ranges. What I like to see is a Free T4 in the top half of the reference range, and a Free T3 at least at the midpoint of the reference range, if not higher.
The third challenge: Even if the TSH is below 2.0, and the Free T4 and Free T3 fall into my optimal range, if you have elevated TPO antibodies you could still be suffering from hypothyroidism symptoms. As I mentioned, elevated antibodies are indicative of Hashimoto’s disease, and you can have symptoms long before the other blood tests show abnormalities. And the good news is that treating people with Hashimoto’s who have otherwise optimal thyroid blood tests may even prevent you from becoming overtly hypothyroid, and lower the antibodies. (An important tip: if you do test positive for Hashimoto’s disease, this means that your first degree relatives — parents, siblings, and children — are at a higher risk of having one of the many diseases that are considered autoimmune in origin. Make sure that you share this information with family members, so they can include it in their medical histories.)
The fourth – and perhaps biggest challenge: Your doctor, insurance company, or HMO may refuse to do anything other than the TSH test. I’ve found that the TSH test alone is not enough to rule out hypothyroidism or Hashimoto’s disease. You can push back with your physician, submit a complaint to your insurance company, or contact the ombudsman at your HMO to argue for the additional tests. But to be honest, if you are meeting with strong resistance, your best option may be not to waste time, and instead, pay out-of-pocket to see a doctor who is already well-versed in diagnosing and managing thyroid and autoimmune issues. (One tip: It’s probably not going to be an endocrinologist. Instead, consider a holistic or integrative physician.) In many states, you can also at least start out by getting the tests done yourself. MyMedLab and HealthCheckUSA are two companies that allow patients to order their own comprehensive thyroid panels, and have blood work done at reputable labs.
Getting Treated
Let’s say that you’ve found a doctor who has run thyroid tests, and your TSH is elevated, or Free T4 and Free T3 are lower than the optimal range. The next step is treatment.
Again, there’s a difference in the way conventional doctors approach this, versus integrative or holistic practitioners. Conventional doctors typically treat with a drug called levothyroxine. Common brand names include Synthroid, Levoxyl, and Tirosint. This is a synthetic form of the T4 hormone. Some people will find that they get full relief of symptoms on a levothyroxine drug, but in my practice, I’ve found that the majority of patients don’t, and need other treatment options. Unfortunately, many endocrinologists and conventional physicians are wedded to levothyroxine-only treatment, and won’t even inform you of your options.
In my practice, I’ve found that many hypothyroid men benefit from the addition of the second thyroid hormone, T3. This can be in the form of a synthetic T3 drug called liothyronine (brand name Cytomel), or a specially compounded, time-released T3 that I prescribe. Some men do better on a natural desiccated thyroid (NDT) drug — these are drugs that have been on the market for almost a century, and are made from the dried thyroid gland of pigs. NDT contains natural versions of T4, T3, and a variety of other cofactors, and seems to work better for some of my patients. Common brands include Armour Thyroid, Nature-Throid, and WP Thyroid. A subset of my patients seem to do best on a T3-only treatment, and typically, for those patients, I find a time-released compounded T3 to work best.
Again, your challenge in treatment may be that your doctor refuses to prescribe a T3 drug, or NDT, or your insurance company or HMO refuses to cover it. Again, you’ll find that integrative and holistic MDs typically follow the approach that the best thyroid drug for you is the one that safely works best for you. And even if you have to pay out of pocket, generic liothyronine and natural desiccated thyroid drugs are generally quite inexpensive. (A tip: if you have to pay a drug co-pay that is more than $15 or $20 for a thyroid drug prescription, make sure you find out the cash price of the drug at the pharmacy. It may actually be less than your co-pay, in which case, it makes sense not to pay through your insurance!)
Periodically, after you start treatment, you’ll need a TSH, Free T4 and Free T3 test to monitor your progress.
The following graphic can be a help in understanding the “optimal” targets, versus the normal reference range, for these tests.
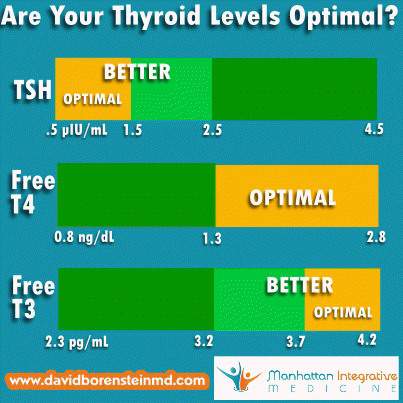
Some Additional Considerations
There are cases where even optimal thyroid treatment — the right drugs and the right blood test levels — may not offer sufficient relief of your symptoms. In this case, I typically look at the remaining symptoms. Are you still losing hair? For my patients, I check ferritin (stored) iron levels, and if they are not in the top 25th percentile of the reference range, I recommend supplemental iron. (Yes, men can be iron deficient too!) Just remember to take any iron supplements at least three to four hours apart from your thyroid medications to avoid any absorption problems. I also frequently check testosterone and dihydrotestosterone (DHT), which is a metabolite of testosterone. High DHT can contribute to hair loss, and there are supplements like saw palmetto and treatments to block the testosterone-DHT conversion process.
If you continue to struggle with fatigue, low sex drive or loss of muscle tone, I typically check testosterone, DHEA-Sulfate (DHEA-S) and estradiol, at minimum. It’s not uncommon to see sub-par levels of these hormones in men who are hypothyroid. In some cases, supplementing with DHEA, or a low dose of prescription testosterone, can get your energy and mojo back.
If you can’t lose weight, that’s when I’ll check your fasting glucose, fasting insulin, leptin and Hemoglobin A1C levels to start. There are supplements like berberine, prescription medications, and dietary changes that can help support your digestive health, and get these levels back on track, and also help prevent insulin resistance or even Type 2 diabetes.
If you have low tolerance for exercise — for example, a few hours of weekend warrior-ing leave you flat on the couch for hours — or you are having unusual sleep patterns like middle of the night waking, early waking, or waking up exhausted even after a good night’s sleep, I also check adrenal function. If levels of your adrenal hormone cortisol are not balanced, there are adrenal herbal formulas that can help get the body’s stress hormones back in balance.
Speaking of stress, one of the things I recommend to all my hypothyroid patients is some sort of daily stress management practice. While your Type A personality may get you ahead in the workplace, it can wreak havoc on your health and hormones, so at least carve out some time each day to take it down a few notches. Typically, something like tai chi, yoga, meditation, breathing, or even an absorbing hobby like woodworking, or relaxing gardening can help lower your heart rate, blood pressure, and stress hormones, and enhance your immune system.
Final Thoughts
In the end, there’s no reason that you should suffer with undiagnosed or poorly treated hypothyroidism. Get in to see your doctor, explain the situation, and be sure to do your best to get the tests and treatments you need. And if your doctor is not cooperative, that’s your sign that it’s time to find someone who will work with you to ensure your optimal health!
About David Borenstein, MD
David Borenstein, MD is the founder of Manhattan Integrative Medicine, an integrative medical practice in New York City, specializing in hormone balance, pain management, and holistic health.

Thanks for the post, very informative. I was first diagnosed with hypothyroidism 3 years ago. and like it said not many people think of men having it. Even Dr’s. My TSH was 209. Needless to say I was feeling pretty miserable. Being a masonry contractor, body aches, pain, and fatigue come with the job. Due to an auto accident not my fault by the way. I was lucky enough to have an informed and knowledgeable Dr. that I was seeing for an after care check up that basically just looked at me and asked if it had ever been checked. I wasn’t obese or really out of my weight range at 206 and 5-10 and being a mason. She just seen things I kind of just blew off, like dry skin and brittle thin hair. I just figured it was from working outside mainly. The more I have looked into it, there aren’t many resources for men on the web for this condition. Glad I found this site, this post and thanks again
Hello,
I’m just wondering how you feel about LDN in addition to thyroid meds for Hashimoto’s? I’ve read some very positive information, including the lowering of thyroid antibodies, decreased brain fog, decreased depression, decreased joint pain and decreased fatigue.
Thank you.
Hi Dana! I came across your article as my own research into Hypothyroidism continues. In 2003, as a 40-yr youngster, unexplained fatigue led to a Dr. appt. On a whim, the Dr. tested my thyroid…quite low. Was very surprised to learn I’d be on Synthroid for life! 16 years later have not missed a dose. My Dad told me after my initial diagnosis that my Mom had hypothyroidism. A number of symptoms on the list applied to me…who knew? Between my thyroid challenge and family history of stroke at a young age, I’ve been very health-conscious into my 40’s and beyond. Look forward to diving into hypothyroidmom.com! Thank you, Dana!
Hi, thank you for this great article. I started with Hyperthyroid and will with a very fast treatment and very little explanation my Thyrois was killed with iode. Now I’m hypothyroid and been taking sintroid since. I went true a few doctors and most only due blood test once a year and I have to say from experience that it’s hard to notice that the med is getting less sufficient. The symptom creeps up very slowly and affects the mental state so we blame everything else. I just got tested last week and my TSH is at 7.3, ooops, so the sintroid got boosted and I’m ask to do another blood test in 3 months( seem a bit long ).
hi I’m a fifty year old man in uk. I’ve been diagnosed as hypothyroid for two plus years now and taking levothyroxine and simvastatin for the entire time and I’ve had a little improvement but not a great deal.
my problem is my doctor will not try any other thyroid drugs and I go to hospital every six months for blood tests and if the levels seem right no change keep taking tablets. and if the levels change then he changes the dose but always the same oils.
on a better note it is nice to see that men with this illness are recognised.
Hi Stephen, It is great to have you at Hypothyroid Mom. I always love hearing from the men with hypothyroidism. My brother has hypothyroidism as well and so it is important that Hypothyroid Mom includes men, women, as well as children. Now looking back I wish that I had picked a different name for my site to be more inclusive but I really started Hypothyroid Mom because I miscarried my baby due to hypothyroidism and so the name made sense.
Just received a blood test with high TSH from my annual physical. Rechecked 30 days later and the TSH is higher. I suffer from fatigue, muscle loss and catch every “bug” that comes within 100 miles of me. As you said, the MD prescribed the typical med. I’ll fill that prescription but want a referral to an Endo for a deeper dive into this. I just can’t see taking a pill for the rest of my life without knowing more. Does this make sense?
Hey brad,
What you’re saying make total sense. I’ve read a book recently written by a practicing physician that explains why patents in this day and age should really become advocates on behalf on their own health.
Don’t just throw everything over the fence and expect someone to take care of all of your problems. Instead, seek out those who understand the problem that you’re facing. If they can’t understand the problem, how are they supposed to fix it? I’d suggest taking that premise and running with it. Quiz your doctor and through your own preparation and homework, hopefully you can meet up with a physician who can help. I’ve heard success stories out there, so its not impossible.